Age-related macular degeneration (AMD) is a common, complex, degenerative condition affecting people aged 50 years and above, causing central vision loss, which results in difficulty to read, drive, or see someone’s face on progression to more advanced stages.
The macula refers to the central portion of the retina. The image one sees is focused by the cornea and lens of the eye onto the center of the retina. Many people with AMD have minimal visual symptoms and may retain good vision indefinitely and a relatively small percentage of people with AMD will lose central vision.
It has multiple risk factors. Family history is another important association, although simply having a blood relative with AMD does not necessarily mean or guarantee that one will definitely develop AMD. Other risk factors for AMD may be modifiable or controllable, including smoking, poor nutritional intake, and high blood pressure.
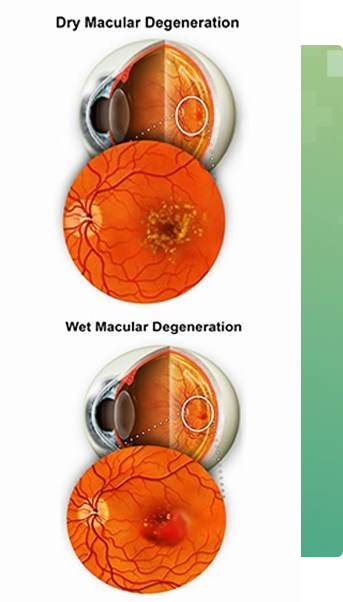
Dry AMD affects about 90 percent of all people with macular degeneration and is characterized by drusen that are visible to the doctor on clinical examination of the macula as small yellow deposit and are the hallmark of AMD. Most people with drusen alone do not have significant visual changes or vision loss. A minority of people with dry AMD will advance to central vision loss due to geographic atrophy, which involves the loss of pigmented cells beneath the macula which normally support and nourish the photoreceptor cells. There is currently no treatment or cure for geographic atrophy, though multiple investigative clinical research trials are going on.
Most people with AMD will retain good central vision in their lifetime, although dry AMD may also gradually progress to an advanced form with atrophy of the macula, limiting central vision.
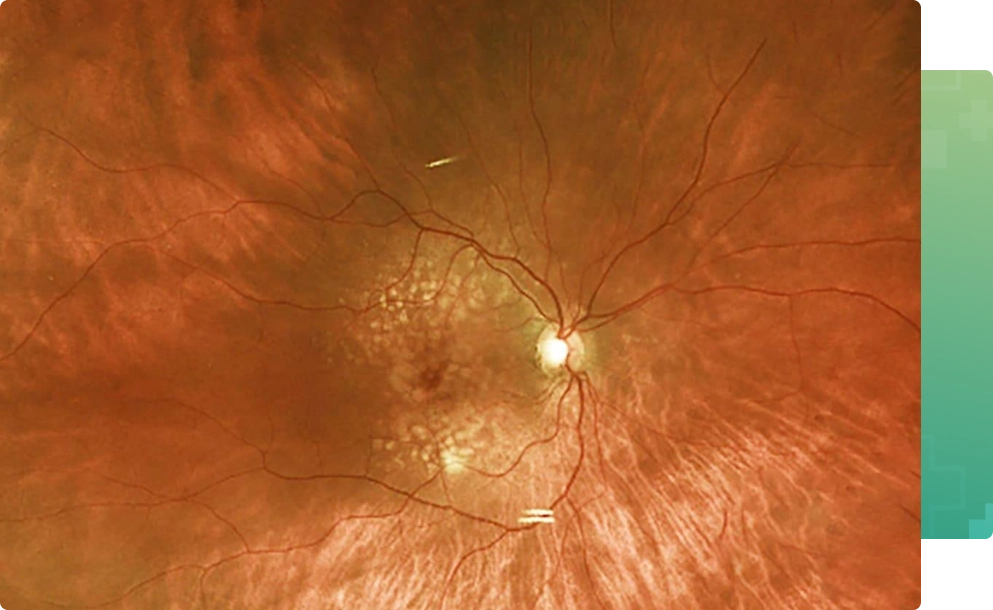
SYMPTOMS – Many people with mild dry AMD have little to no visual symptoms. Some people, however, will experience some side effects, like:
Vision loss associated with dry AMD is usually gradual or slow. Because AMD affects the macula, the symptoms are typically related to central vision tasks such as reading or driving. Peripheral vision is typically preserved.
MANAGEMENT OF DRY AMD – Patients with dry AMD are followed up at regular intervals to look for the progression of AMD from the dry to the wet variety.
Wet AMD affects only about 10 percent of people with macular degeneration, but accounts for the majority of central vision loss in those who have macular degeneration.
The word “wet” implies leakage and bleeding in the macula due to abnormal blood vessels (choroidal neovascularization) that may develop spontaneously in AMD. If left untreated, it results in severe central vision loss due to permanent scarring of macula. While patients may progress to legal blindness, it is important to realize that AMD affects central vision – it typically does not lead to total loss of vision. Fortunately, there are new treatments available for those with wet AMD.
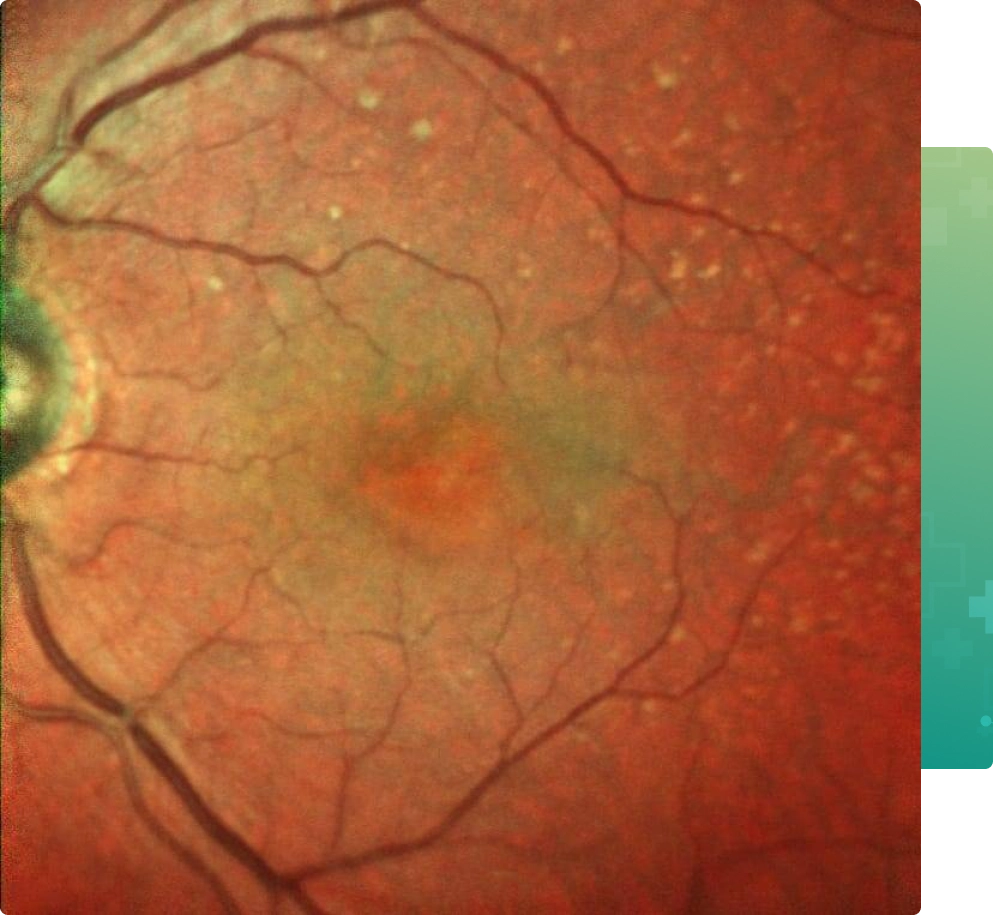
SYMPTOMS – Patients with wet AMD often have pronounced symptoms, including:
Occasionally, people may not be aware of these visual changes as their other eye may be functioning normally. Therefore, it is important to test vision in each eye separately by covering one eye at a time when checking vision.
Management of Wet AMD – This includes the use of intravitreal antivegf injections like Lucentis, Razumab, Eylea, Avastin and Pagenax and laser treatment modalities like thermal laser, transpupillary thermotherapy (TTT) or photodynamic therapy (PDT).
At Narayana Nethralaya, “Quality of Care” and “Patient Safety” is our priority. Concern for our patients’ well being is at the core of what we do, and what drives us. All 4 units of Narayana Nethralaya are NABH Accredited – the highest national recognition for quality in patient care and safety. Our Retina team help patients make an informed treatment choice on the type of treatment and surgery that is best suited for their lifestyle. We have an exclusive counseling team to address any doubts or questions that people may have about Retina treatment options and procedures.
