Diabetic retinopathy occurs secondary to deterioration of blood vessels in the retina as a complication of diabetes mellitus. The breakdown of retinal blood vessels which occurs in diabetic retinopathy may result in fluid leaking into the center of the retina (macular edema) or abnormal blood vessels formation on the surface of the retina (neovascularization) which can bleed and scar resulting in loss of central and possibly peripheral vision.
There are two major types of diabetic retinopathy: non-proliferative and proliferative.
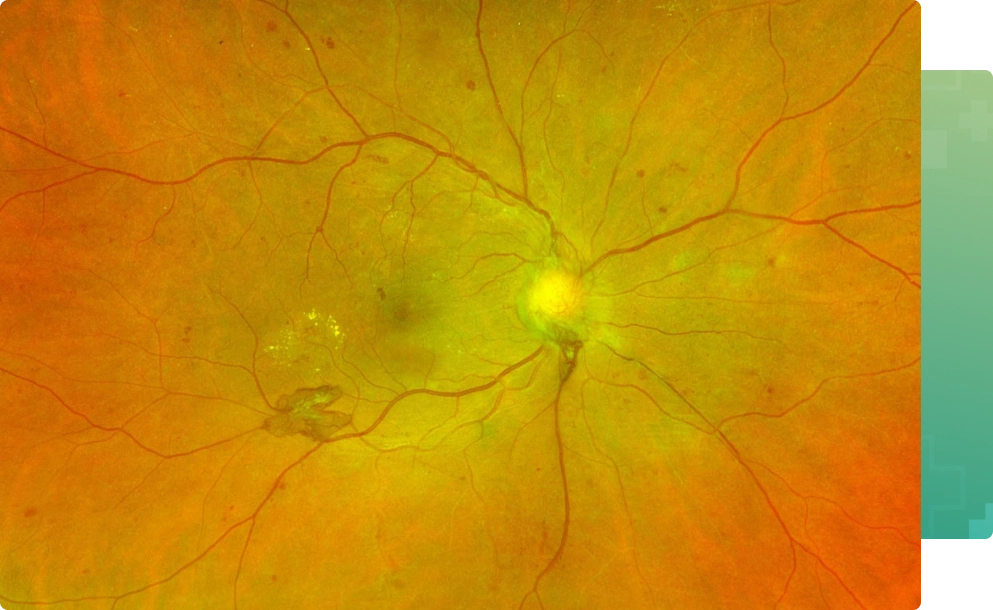
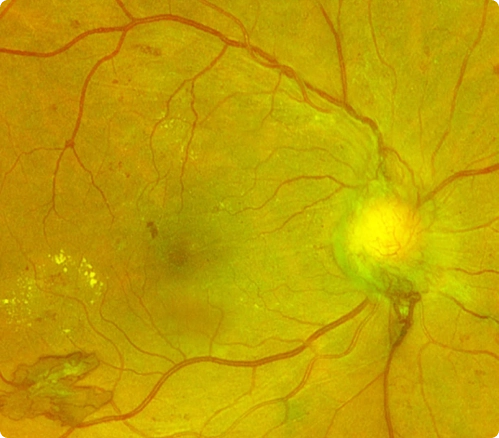
The longer the duration of diabetes mellitus, the more likely they will develop diabetic retinopathy. After 25 years, nearly all patients with diabetes mellitus will show some signs of retinopathy. The severity is also related to blood glucose (sugar) control. Keeping blood glucose levels under control reduces the degree and rate of progression of diabetic retinopathy and other diabetic complications in the body.
Medicines injected into the eye such as anti-VEGF drugs (eg. Lucentis, Razumab, Eylea, Avastin and Pagenex) and steroids (eg. Triamcinolone and Ozudex) are now commonly used to treat diabetic macular edema and some of the proliferative manifestations of the condition. Both anti-VEGF and steroid medications have been proven in large-scale studies to be highly effective in reducing macular edema and improving vision.
The anti-VEGF agents are generally considered as the first line therapy for treating most cases. Repeat injections may be necessary for long-term control of the retinopathy.
The injections are performed in the operation theatre using topical anaesthetic eye drops. They are very well tolerated and complications like infections are rare. Steroid injections may be associated with elevated eye pressure.
Laser photocoagulation is a well known treatment for diabetic retinopathy, wherein laser is delivered as a split-second burst of intense light energy to treat the leaky retinal blood vessels or promote shrinkage of abnormal blood vessels (neovascularization) which has been proven in large clinical trials to significantly reduce the risk of both moderate and severe vision loss in people with diabetic retinopathy.
Laser photocoagulation is performed in the office setting with the patient seated in front of the laser unit. The eye is anesthetized with drops and a contact lens may be placed on the eye to focus the laser-aiming beam. Patient may sense bright flashes of lights and occasionally a pinching sensation, although most of them will have no sensation of the laser at all. Some people may experience discomfort during laser procedure, but is generally well-tolerated.
People with diabetic retinopathy may require vitrectomy surgery in an operating room setting. A vitrectomy is performed when there is bleeding or retinal traction that is causing loss of vision in advanced diabetic retinopathy. In this surgical procedure, small instruments are inserted into the eye under microscopic visualization to remove the vitreous hemorrhage and any scar tissue . Endo-Laser photocoagulation may be performed during the surgery, and in some cases, a gas bubble or silicone oil may be injected to hold the retina in position .The prognosis of vitrectomy surgery depends upon the status of the underlying diabetic retina.