Narayana Nethralaya has fully equipped state of art vitreo retinal surgical suites in each of its branches. The surgeries are performed for a variety of retinal disorders like retinal detachment, advanced diabetic eye disease, vitreous hemorrhage, endophthalmitis, macular hole and epiretinal membrane using the latest small gauge micro incisional vitrectomy system (MIVS). The institute also boasts of having the 3D Ngenuinity visualisation system which allows the surgeon to perform a heads-up vitreoretinal surgery. Also, scleral buckle surgery and pneumatic retinopexy are routinely performed for the management of rhegmatogenous retinal detachment. Complications following anterior segment surgeries like dislocated nucleus and intraocular lens dislocation are managed with the fixing of the scleral fixated or iris-claw intraocular lenses.
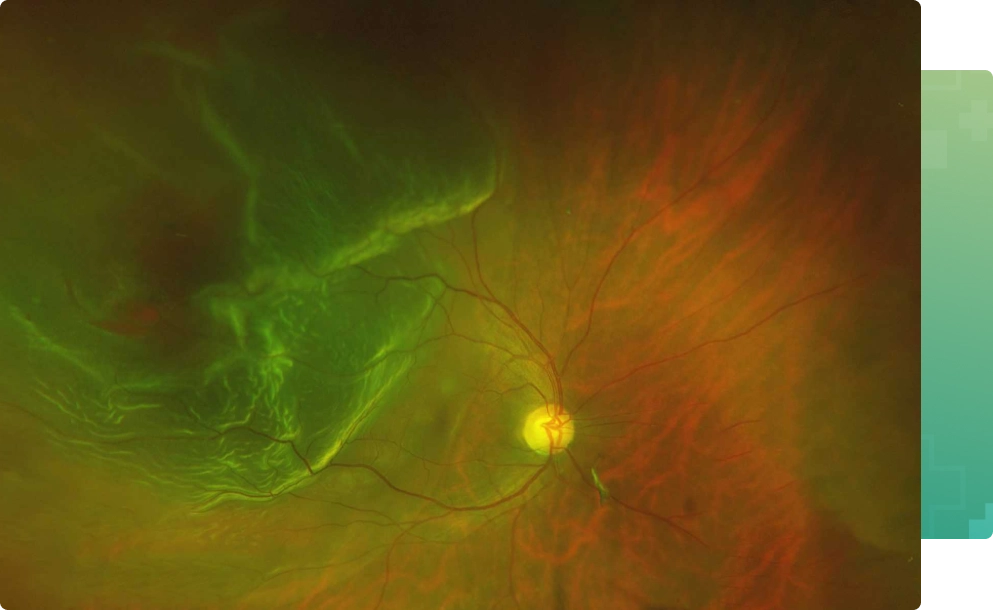
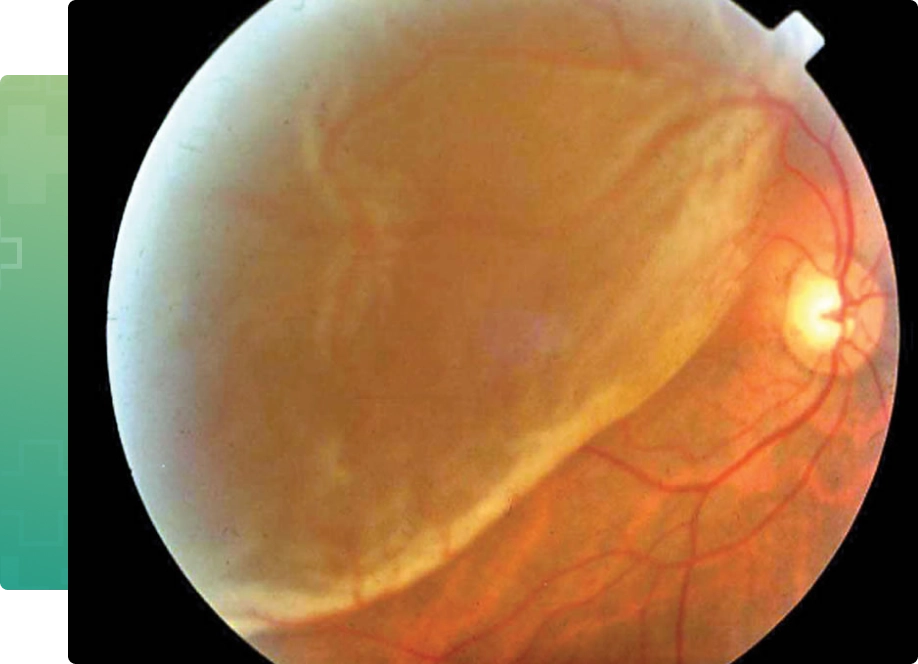
A retinal detachment is a separation of the retinal layers. Over time, retinal detachment will lead to progressive loss of peripheral and, eventually, central vision. Left untreated, total and permanent loss of sight eventually occurs in most cases.
A rhegmatogenous type of retinal detachment which is the most common type is caused by a break, tear or hole in the retina, allowing fluid from the vitreous cavity of the eye to go under the retina, detaching it from the eye wall. Retinal tears and associated detachments of the retina are often spontaneous and unpredictable events. While detachment can arise following trauma, it is usually caused by separation of the vitreous gel from the retina. Over time as we age, the vitreous gel liquefies. It eventually collapses upon itself and separates from the surface of the retina (posterior vitreous detachment). During or shortly after this event, a retinal tear can occur as a result of the gel pulling on the thin retinal tissue.
Risk factors for developing retinal tears and detachment include myopia (near-sightedness), particularly thin patches within the peripheral retina (lattice degeneration), family history, previous eye surgery, and trauma.
The rate of progression of a retinal detachment can vary from days to weeks depending on many factors such as patient age as well as the size and the number of retinal tears.
Symptoms of vitreous detachment, retinal tear, and retinal detachment may coexist and include:

While BRVO cannot be cured, there are effective treatments that can help patients maintain or improve their visual outcome by reducing the associated macular edema. Treatment options include intravitreal injection (injection of medicine into the eye) and laser.
Intravitreal injection of vascular endothelial growth factor (VEGF) inhibitors such as Lucentis (FDA approved), Eylea (FDA approved), and Avastin (used off-label) or steroids such as triamcinolone and Ozurdex (FDA approved) can help maintain or improve vision.
Laser is sometimes used to treat macular edema but is now considered a second-line treatment for most cases based on visual outcomes and limitations. For instance, if there is significant hemorrhage in the retina, laser cannot be performed until the hemorrhage resolves spontaneously, which takes few months.
In response to a BRVO, some patients will develop an abnormal growth of fragile new blood vessels (retinal neovascularization) on the surface of the retina months or years after initial diagnosis. These blood vessels generally do not have any associated symptoms unless they rupture and bleed. In general, rupture is spontaneous and unpredictable, and if there is a significant amount of hemorrhage into the vitreous cavity of the eye, vision can be dramatically reduced. Although the blood may resolve spontaneously in some cases, it can take weeks or months depending on the severity. If neovascularization is detected on a follow-up office visit, laser can be administered to shrink the abnormal fragile vessels in order to minimize the risk of vitreous hemorrhage and vision loss. Laser does not guarantee that there will be no future haemorrhaging, but it does significantly lower this risk. Occasionally if there is a very severe or persistent (non-clearing) vitreous hemorrhage, vitrectomy surgery may be warranted to remove the blood.